Negative Pressure Wound Therapy (NPWT), or wound vacs, can be incredibly effective — until the wound isn’t straightforward.
In home health, we don’t always get clean, granulating wounds with perfect orders. We walk into homes with mixed tissue, questionable eschar, exposed structures, fragile periwound skin, and orders that don’t quite match what we’re seeing.
This is where understanding eschar, black foam vs white foam, and why each one exists becomes critical — not just for wound healing, but for patient safety and license protection.
First: Let’s Talk About Eschar (Because This Is Where Things Go Wrong)
Eschar is dead, necrotic tissue. It’s typically:
- Black or dark brown
- Leathery or hard
- Dry or firmly adhered
Key rule that does NOT change:
👉 NPWT should not be applied directly over hard, dry, stable eschar.
A wound vac works by removing fluid, reducing bioburden, and promoting granulation — but eschar is non-viable tissue. Suction over stable eschar does not magically convert it into healthy tissue and can actually cause harm.
When eschar becomes complicated:
- Eschar with lifting edges
- Eschar with drainage underneath
- Mixed wounds (eschar + slough + granulation)
- Surgical wounds that have partially necrosed
- Traumatic wounds evolving over time
These are the scenarios where nurses get stuck — and where foam choice matters.
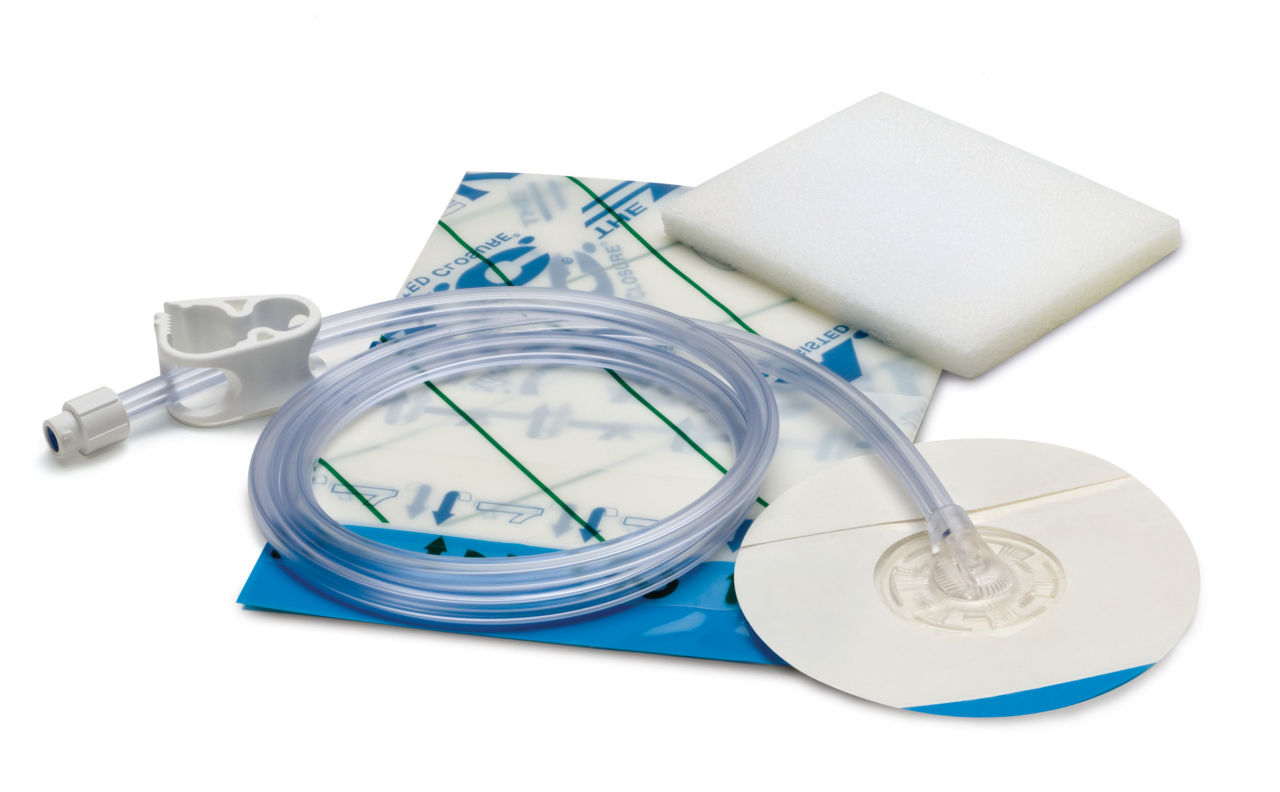
Black Foam vs White Foam: They Are NOT Interchangeable


4
Black Foam (Polyurethane Foam)
What it does well:
- Promotes aggressive granulation
- Excellent fluid removal
- Helps reduce wound size faster
What it’s best for:
- Granulating wounds
- Deep cavities with healthy tissue
- Wounds with moderate to heavy exudate
What it does NOT do well:
- Protect delicate structures
- Sit safely against exposed tendon, bone, or vessels
- Tolerate fragile or painful wound beds
Black foam is more porous and “grabby.” That’s great for granulation — terrible for exposed structures or friable tissue.
White Foam (Polyvinyl Alcohol Foam)
What it does well:
- Protects delicate structures
- Provides gentler pressure
- Reduces pain during therapy and removal
What it’s best for:
- Exposed tendon, bone, or vessels
- Fragile wound beds
- Tunneling or undermining
- Pain-sensitive patients
- Areas near organs or grafts
What it does NOT do well:
- Aggressive granulation
- Heavy drainage management on its own
White foam is denser and less porous. It’s protective, not aggressive.
So What About Eschar + Wound Vac?
This is where clinical judgment — and documentation — matters most.
Scenario 1: Stable, Dry, Intact Eschar
❌ Do NOT place NPWT
- No black foam
- No white foam
- No suction
This requires provider notification, not creative wound care.
Scenario 2: Lifting Eschar with Drainage or Mixed Tissue
This is where wound vacs may come into play after provider involvement.
Common safe approaches (order-dependent):
- Conservative debridement by qualified provider
- Enzymatic or moisture-based softening first
- NPWT applied only to viable tissue
- Protective interfaces used between foam and questionable areas
👉 White foam or a contact layer is often required here to avoid trauma.
Scenario 3: Exposed Tendon or Bone After Eschar Breakdown
This is a white-foam situation, full stop.
Black foam directly on exposed structures can:
- Cause tissue damage
- Increase pain
- Increase risk of bleeding
- Create legal and clinical risk for the nurse
White foam acts as a buffer, allowing negative pressure therapy to continue safely.
The Hidden Risk: When Orders Say “Wound VAC” — But Don’t Specify Foam
This happens constantly in home health.
If an order simply says “Apply wound vac” without specifying:
- Foam type
- Contact layers
- Pressure settings
- Structure protection
👉 You are still responsible for safe application.
That means:
- Assessing tissue type
- Identifying exposed or at-risk structures
- Using white foam or protective layers when indicated
- Notifying the provider when the wound presentation doesn’t match the order
Documentation That Protects You
When dealing with eschar and NPWT, your note should clearly show:
- Tissue types present (eschar, slough, granulation)
- Stability of eschar (intact vs lifting vs draining)
- Presence or absence of exposed structures
- Foam selection and rationale
- Provider notification when indicated
- Patient tolerance and pain response
Avoid vague language like “wound looks okay.”
Be specific. Be defensible.
Bottom Line for Home Health Nurses
- Eschar ≠ automatic wound vac
- Black foam = aggressive granulation
- White foam = protection and safety
- Foam choice is a clinical decision, not just a supply issue
- When in doubt, pause, protect, and escalate
Understanding why we choose black vs white foam — especially in complicated wounds — is what separates task-based wound care from skilled nursing judgment.
If you want a step-by-step framework for handling no-order wound scenarios, mixed tissue wounds, and advanced NPWT decision-making, that’s exactly what I’m building next.
Because home health wounds are rarely simple — and nurses deserve guidance that matches reality.
check out my books i wrote related to this topic
How These Two Books Work Together
Home health wound care rarely comes to us fully ordered, neatly staged, and perfectly aligned with what’s happening in the patient’s home.
That reality is exactly why these two books exist — and why they are designed to be used together, not interchangeably.
Each book solves a different but connected problem that home health RNs face every day.
Home Health Wound Care Without Orders
A Field Manual for RN Assessment, Interim Treatment, and Provider-Approved Regimens
This book begins before orders exist.
It is built for the moments when:
- A wound is present, but no wound care orders were sent
- The hospital orders are vague, outdated, or unsafe
- The wound presentation does not match the paperwork
- You must assess, stabilize, and advocate — without practicing outside your scope
This field manual focuses on:
- RN-level wound assessment and classification
- Identifying tissue type, exudate, periwound risk, and infection concerns
- Safe interim treatment principles while awaiting provider input
- How to communicate clear, defensible wound recommendations to providers
- Documentation language that protects your license and supports Medicare scrutiny
This is the decision-making book.
It teaches you how to think through complex wounds when you are the first — or only — clinician seeing the wound in the home.
A Home Health RN’s Field Guide to NPWT Dressing Changes and Medicare-Defensible Documentation
Field-Tested Guide for Home Health RNs
This book begins after NPWT enters the picture.
It is designed for situations where:
- A wound vac is ordered, but the wound is complicated
- The foam choice, seal method, or application technique matters
- You are troubleshooting leaks, pain, tunneling, eschar, or mixed tissue
- Documentation must clearly justify skilled nursing involvement
This guide focuses on:
- NPWT dressing changes in real home environments
- Black foam vs white foam decision-making
- Protecting exposed structures and fragile tissue
- Bridging, undermining, and seal-failure troubleshooting
- Medicare-defensible NPWT documentation that shows skill — not just task completion
This is the execution and documentation book.
It teaches you how to safely carry out advanced NPWT while clearly proving skilled need.
Why Both Books Matter
In real home health practice, wound care does not follow a straight line.
A nurse may:
- Assess a wound without orders on Monday
- Advocate for a regimen on Tuesday
- Receive NPWT orders on Thursday
- Manage complex NPWT scenarios for weeks afterward
One book covers the clinical thinking and advocacy before orders.
The other covers the technical execution and documentation after NPWT begins.
Together, they create a complete framework:
- Assess safely
- Treat within scope
- Advocate clearly
- Execute confidently
- Document defensibly
Who These Books Are For
These guides are written for:
- Home health RNs who practice independently in the field
- Nurses managing complex wounds with limited immediate provider access
- Clinicians who want clear reasoning, not generic wound care rules
- Nurses who care about license protection and Medicare compliance
They are not academic wound texts.
They are field manuals — written by a home health RN, for home health reality.
The Bottom Line
You should never feel forced to choose between:
- Doing what the wound needs
- Staying within your scope
- Protecting your license
These books exist to help you do all three — clearly, safely, and defensibly.
Used together, they reflect the full lifecycle of real-world home health wound care — from first assessment to advanced NPWT management — exactly as it happens in the field.

Leave a comment